New Research Reveals How Mast Cells in the Gut Trigger Severe Food Allergy and Anaphylaxis
A major new study published in Science has uncovered an important mechanism behind severe food allergy reactions and anaphylaxis. Researchers discovered that specialised immune cells in the gut — mast cells — can trigger life-threatening allergic reactions using powerful inflammatory chemicals, even before allergens enter the bloodstream.
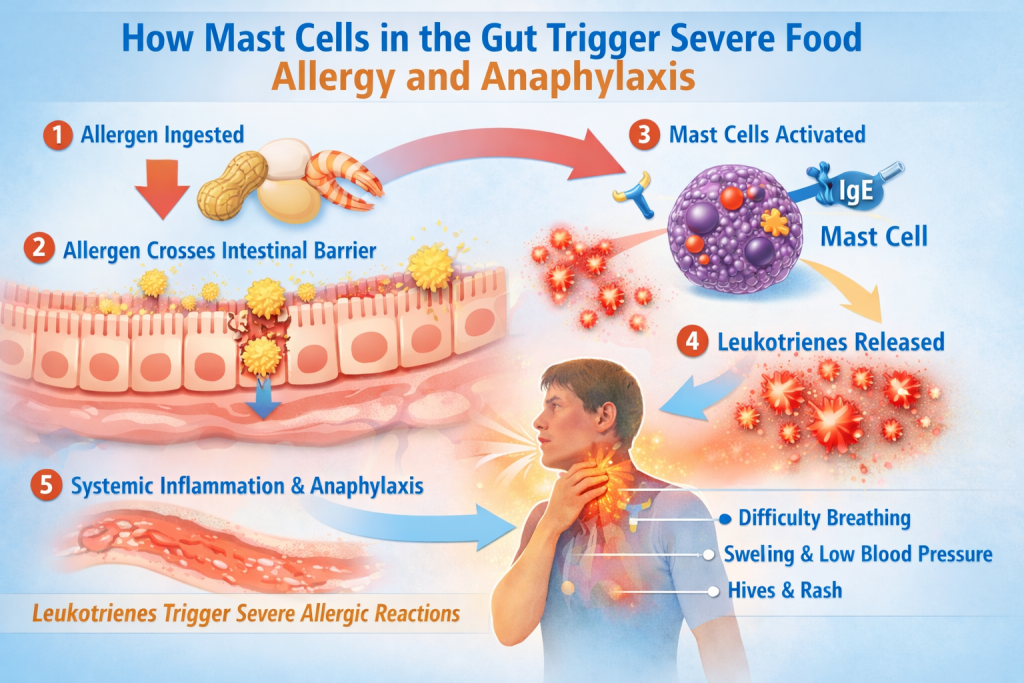
Mast cells in the intestinal lining activate after food allergen exposure, releasing leukotrienes that can trigger severe allergic reactions and anaphylaxis.
The full research paper is available free via PubMed Central, offering new insight into why eating certain foods can cause sudden and severe reactions in some individuals. The official version of record is available on the Science website (DOI: 10.1126/science.adp0246)
What Is Anaphylaxis?
Anaphylaxis is the most serious type of allergic reaction. It can develop within minutes and requires urgent medical treatment with adrenaline (epinephrine).
Common symptoms include:
– Difficulty breathing
– Swelling of the throat or tongue
– A sudden drop in blood pressure
– Dizziness or fainting
– Skin reactions such as hives (urticaria)
Food allergy is one of the leading causes of anaphylaxis, particularly in children and young adults.
The Key Discovery – Intestinal Mast Cells Drive Severe Food Allergy
Mast cells are immune cells that act as the body’s early warning system. They play a central role in IgE-mediated allergic reactions.
This new research shows that mast cells located in the intestinal lining behave differently from those in the skin or lungs.
Intestinal mast cells:
– Sit directly within the gut’s surface layer
– Interact closely with surrounding intestinal epithelial cells
– Produce relatively low amounts of histamine
– Produce high levels of inflammatory chemicals called leukotrienes
This finding suggests that food-triggered allergic reactions follow a distinct biological pathway, different from injected or skin-triggered allergies.
Leukotrienes – A Hidden Driver of Food-Induced Anaphylaxis
Leukotrienes are powerful inflammatory molecules already known to play a major role in asthma.
The study found that during food-induced allergic reactions:
– Leukotrienes are key drivers of systemic anaphylaxis
– Blocking leukotriene production prevented severe reactions in experimental models
– Standard antihistamines were less effective for food-triggered reactions
By contrast, allergic reactions caused by injected allergens relied more heavily on histamine release.
How Food Allergy Reactions May Start in the Gut
Researchers propose the following sequence in severe food allergy:
-
A food allergen is eaten
-
It crosses the intestinal barrier
-
Mast cells release leukotrienes
-
Inflammation spreads throughout the body
In short, anaphylaxis may begin locally in the intestine before becoming systemic.
Why Some Food Allergies Are More Severe Than Others
The findings may help explain why some people experience mild symptoms, while others develop life-threatening anaphylaxis.
Severity may depend on:
– The number of mast cells present in the gut
– How strongly these cells produce leukotrienes
– The integrity of the intestinal barrier
– Signals from surrounding gut tissues that shape immune responses
Understanding these mechanisms could help identify patients at higher risk of severe reactions.
New Possibilities for Food Allergy Treatment
An exciting aspect of this research is that leukotriene-targeting medications already exist and are widely used for asthma management.
In laboratory models:
– Blocking leukotriene pathways significantly reduced severe reactions after allergen exposure
– Combined approaches targeting both histamine and leukotrienes may offer improved protection
However:
– Most findings are currently based on animal studies
– Human clinical trials are required
– Current clinical advice remains unchanged
People with diagnosed severe food allergy must continue to:
– Strictly avoid trigger foods
– Carry adrenaline auto-injectors at all times
– Seek urgent medical help if symptoms occur
Why This Food Allergy Research Matters
Food allergies are increasing worldwide. Severe reactions place a major burden on:
– Patients and families
– Schools and childcare settings
– Healthcare systems
This discovery highlights the gut immune system as a critical control centre for allergic responses — not merely a site of digestion.
Understanding how intestinal mast cells and leukotrienes drive anaphylaxis could transform:
– Risk prediction
– Preventive strategies
– Future food allergy treatments
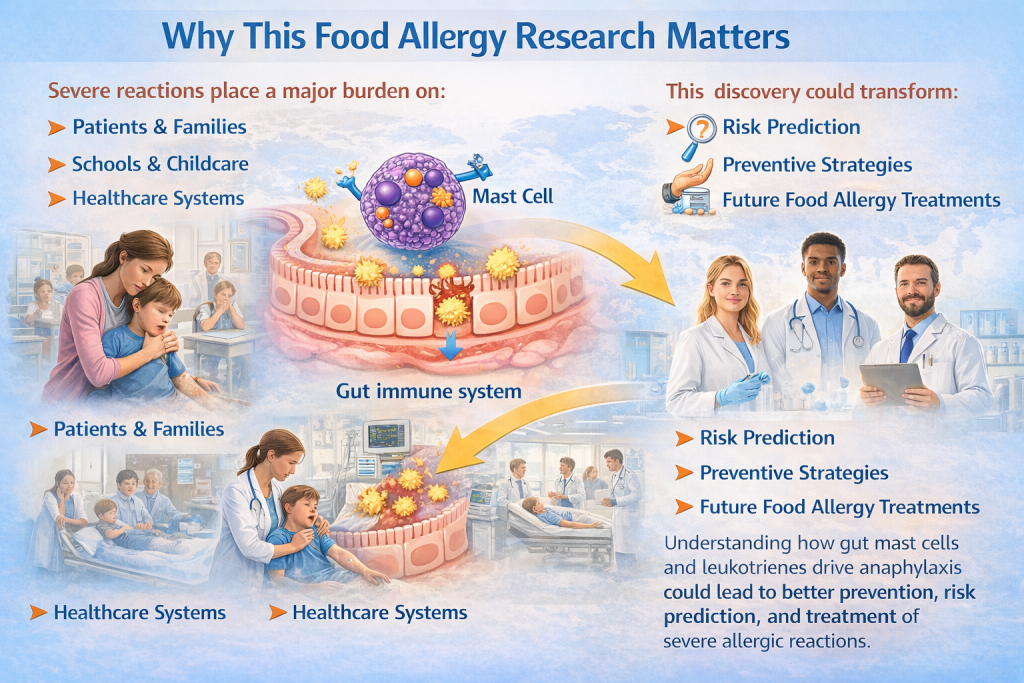
Why food allergy research matters, showing the burden of severe allergic reactions and how understanding gut mast cells may improve risk prediction and treatment.
By revealing the role of intestinal mast cells and leukotrienes, scientists have opened a promising new path towards better prevention, risk prediction, and treatment of anaphylaxis.
Keywords: food allergy, anaphylaxis, gut immune system, mast cells, leukotrienes, severe allergic reaction, food allergy research, intestinal immune response, allergy treatment and research